Healthcare systems worldwide are under immense pressure to balance operational efficiency with delivering timely, personalised patient care. Traditional appointment booking methods, primarily phone calls or online forms, often lead to bottlenecks, staff overload, and suboptimal patient experiences. Voice assistants for healthcare appointment booking are changing this dynamic. These AI-powered systems use natural language processing (NLP) to engage with patients via speech, allowing them to schedule, modify, or cancel appointments using simple spoken commands, 24/7, without call queues.
| Quick Answer : Voice assistants streamline healthcare appointment booking by using natural language processing (NLP) to let patients schedule, modify, or cancel appointments via voice commands — 24/7, without call queues. Integrated with EHR and CRM systems via FHIR APIs, they reduce no-show rates by up to 72%, cut cost-per-booking from $8–15 to $1–3, and free staff from up to 38% of administrative scheduling workload. |
Voice scheduling is one component of a broader AI in healthcare transformation that is reshaping how hospitals operate, engage patients, and deliver care.
Whether it is booking a consultation with a general practitioner or scheduling a specialised diagnostic test, voice assistants offer real-time interaction that mirrors human-like conversation. This guide covers how they work, how they integrate with hospital systems, what results leading hospitals are seeing, and how the technology is evolving.
Traditional vs. AI-Powered Healthcare Appointment Booking: A Full Comparison
Before evaluating voice assistants, it helps to understand exactly what they replace. The table below compares traditional phone-and-form scheduling against AI-powered voice booking across the dimensions that matter most to hospital operations teams.
Availability. Traditional booking is limited to business hours and staff capacity. Voice assistants operate 24/7, handling simultaneous requests without hold times.
Cost per booking. Manual scheduling typically costs $8–15 per appointment when factoring in staff time, phone infrastructure, and error correction. Voice AI reduces this to $1–3 per booking by automating the entire workflow.
No-show management. Phone-based reminders are inconsistent and resource-intensive. Voice assistants deliver multi-touch, personalised reminders at optimal intervals (72 hours and 24 hours before the appointment), with one-tap confirm or reschedule options, cutting no-show rates by up to 72%.
Language support. Traditional call centres require multilingual staff, which is expensive and hard to scale. Voice assistants handle dozens of languages natively using NLP models, making healthcare access equitable across diverse patient populations.
Scalability. Adding call centre capacity means hiring, training, and managing more staff. Voice AI scales instantly during peak demand (flu season, vaccination drives, outbreaks) without additional headcount.
Data capture. Manual booking often results in incomplete or inaccurate patient records. Voice assistants capture structured data (patient ID, appointment type, preferred provider, insurance details) and write it directly to the EHR and scheduling system in real time.

How Do Voice Assistants Work for Healthcare Scheduling?
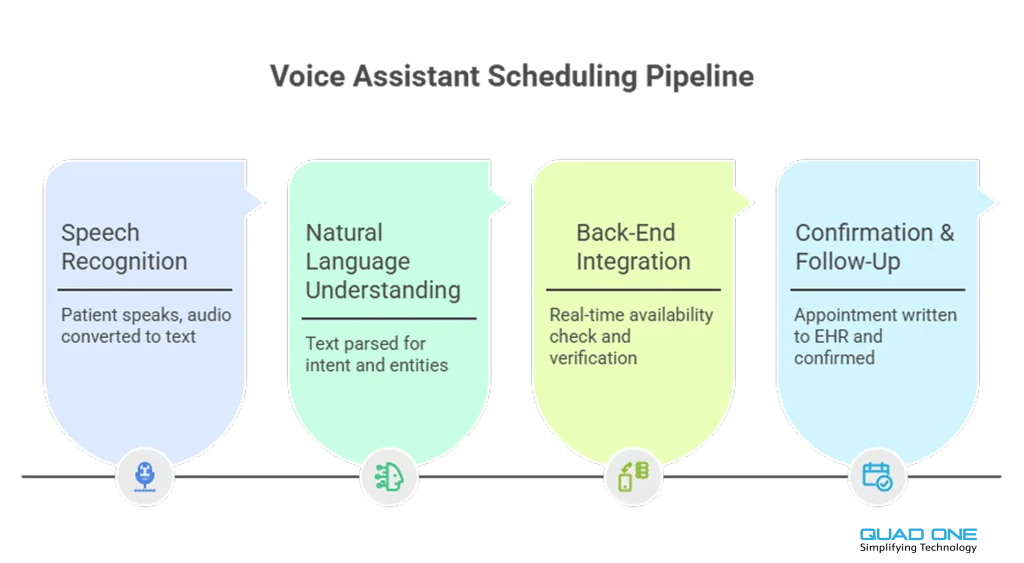
A voice assistant for healthcare scheduling operates through a four-stage pipeline that converts spoken patient input into a confirmed appointment record inside the hospital’s systems.
Stage 1: Speech Recognition. The patient speaks naturally (“I need to see Dr. Patel next Thursday afternoon”). Automatic speech recognition (ASR) converts the audio to text. Modern ASR models handle accents, medical terminology, and background noise with accuracy rates above 95%.
Stage 2: Natural Language Understanding (NLU). The NLU engine extracts intent (book, reschedule, cancel) and entities (provider name, date, time preference, appointment type). It disambiguates: “next Thursday” becomes a specific calendar date; “afternoon” maps to available slots between 12:00 and 17:00.
Stage 3: Back-End Integration. The system queries the scheduling engine via FHIR APIs to check real-time provider availability, patient eligibility, and insurance coverage. If the requested slot is unavailable, the assistant proposes alternatives ranked by proximity to the patient’s preference.
Stage 4: Confirmation and Follow-Up. The assistant confirms the booking, writes the appointment to the EHR, and triggers a confirmation message through the patient’s preferred channel (voice callback, SMS, WhatsApp, email). Automated reminder sequences are scheduled (72h + 24h) with one-tap reschedule links.
Technical Integration: Connecting Voice AI to Hospital Systems
For hospital administrators and Health IT professionals, the most significant advantage of voice assistants is their ability to integrate securely and effectively with back-end infrastructure. Successful implementations typically include EHR and scheduling system integration to enable real-time availability checks and booking updates, Natural Language Understanding (NLU) capabilities to support multilingual patient interaction, omni-channel deployment via smart devices, mobile apps, and IVR phone systems, and FHIR-compatible APIs for standardised data exchange.
Voice assistants use FHIR (Fast Healthcare Interoperability Resources) APIs to securely exchange standardised healthcare data. These APIs enable voice systems to access appointment slots, patient records, and provider availability through consistent formats, reducing integration time by 30–40% compared to custom approaches.
When voice scheduling is connected to an AI hospital CRM, the booking data feeds directly into patient engagement workflows: automated pre-visit prep, post-visit follow-ups, and feedback collection all trigger from the same appointment event.
HIPAA compliance is non-negotiable. Voice data must be encrypted during transmission and at rest. Patient identity verification (date of birth, MRN, or biometric voice print) must precede any access to Protected Health Information. Audit logs must record every interaction. Leading implementations use end-to-end encryption and store voice recordings only when explicit patient consent is captured.
Real-World Results: How Leading Hospitals Use Voice Assistants
United States
Leading healthcare systems including Kaiser Permanente, Cleveland Clinic, Providence Health, and Mass General Brigham have implemented voice assistants for scheduling. Key technology providers include Microsoft Healthcare Bot, Google Health AI, and Amazon Comprehend Medical. Northeast Medical Group implemented a voice-first scheduling system and experienced significant improvements in booking completion rates and staff time savings.
Healthcare organisations like Cleveland Clinic and Mayo Clinic are now leveraging advanced voice capabilities to not only schedule appointments but also help prioritise urgent cases and suggest appropriate care levels based on symptom description.
India
Apollo Hospitals deployed an Alexa-based voice skill linked to its internal scheduling systems. Later enhanced with multilingual support through WhatsApp and mobile platforms, Apollo reported a 49% increase in appointment bookings, particularly from regions with limited digital literacy. Their latest update added support for 8 regional languages, allowing them to reach over 80% of the Indian population in their native language.
In India, the combination of voice assistants and WhatsApp patient communication offers massive reach, especially in semi-urban and rural areas where voice-first interaction is the natural digital entry point.
Middle East
Medcare Hospitals in the UAE launched an AI assistant capable of handling bookings, cancellations, and rescheduling in real time. With Arabic-English bilingual capabilities and backend system integration, the assistant significantly improved both patient satisfaction and staff productivity. The UAE Ministry of Health has since established new standards for voice assistant implementation, making it part of their 2025 healthcare digitisation initiative.
These regional case studies share a common success factor: seamless integration with existing hospital systems (scheduling engines, CRMs, EHRs) combined with the ability to deliver a responsive, voice-enabled interface localised for the patient population.
How Do Voice Assistants Reduce No-Show Rates?
No-shows are one of healthcare’s most expensive blind spots. In the US alone, missed appointments are estimated to cost providers more than $150 billion annually. Voice assistants attack no-shows through three mechanisms.
Multi-touch, personalised reminders. Unlike generic SMS blasts, voice assistants deliver conversational reminders at optimal intervals. They call the patient, confirm intent, and offer one-tap rescheduling if the patient cannot make it. The conversational format drives higher engagement than text-only reminders.
Predictive no-show identification. AI models analyse historical attendance patterns, demographic factors, and appointment characteristics to flag high-risk patients. These patients receive enhanced engagement: additional reminder touchpoints, transportation assistance information, and proactive outreach from staff.
Instant waitlist backfill. When a patient cancels or reschedules, the voice assistant immediately contacts waitlisted patients with matching availability preferences and books the open slot in real time. This preserves clinic capacity that would otherwise be lost.
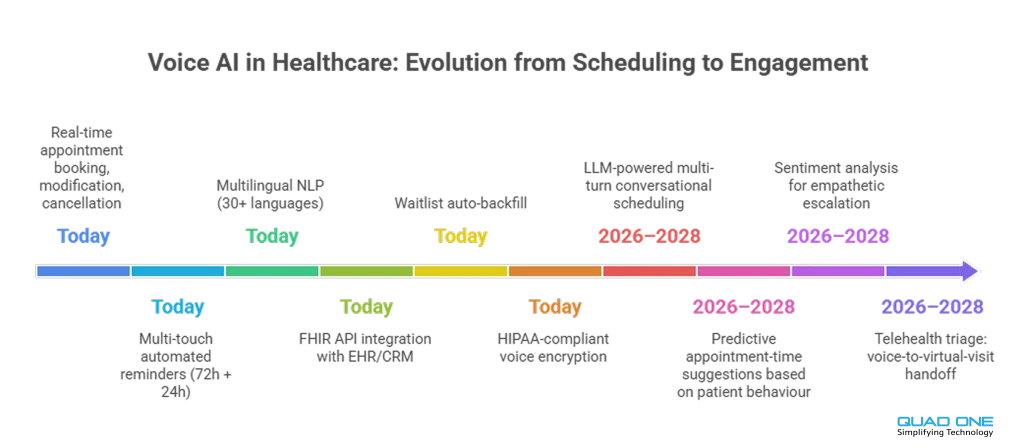
The Future of Voice AI in Healthcare Scheduling
The latest voice assistants are transcending basic scheduling functionality. Emerging capabilities include:
Large Language Models (LLMs) that enable more natural, context-aware conversations with patients. Instead of rigid slot-filling dialogues, the assistant can handle complex multi-turn requests (“I need to see my cardiologist sometime next week, but not Tuesday, and I’d prefer morning”) in a single conversational flow.
Predictive analytics that suggest optimal appointment times based on historical data and patient preferences. Systems at MetroHealth and Johns Hopkins are already using this to reduce scheduling friction.
Sentiment analysis that detects patient stress or confusion and adjusts responses accordingly, slowing down, simplifying language, or escalating to a human agent.
Integration with telehealth platforms for seamless virtual care transitions is accelerating. Learn more about Quad One’s AI telemedicine solution and how voice-booked appointments can transition between in-person and virtual modalities based on clinical need.
The next generation of voice solutions will not only streamline bookings but also support triage, medication adherence, and chronic disease management, turning the scheduling touchpoint into a broader patient engagement channel.
Implementation Playbook: Getting Started with Voice Scheduling
For hospital executives, innovation leaders, and health IT professionals looking to implement voice assistants, the following action steps provide a structured path to deployment:
Step 1: Audit current scheduling inefficiencies. Quantify call volumes, average hold times, no-show rates, cost-per-booking, and staff time spent on scheduling. This establishes the baseline for ROI measurement.
Step 2: Define integration requirements. Map the voice assistant’s data needs: which EHR fields, scheduling engine APIs, and patient identity verification methods are required. Confirm FHIR API availability from your EHR vendor.
Step 3: Start with a single high-volume use case. New patient appointments or follow-up scheduling are ideal pilots. Limit scope to one department or clinic to prove value before expanding.
Step 4: Configure multilingual and omni-channel support. Prioritise the languages spoken by your patient population. Deploy across the channels patients already use: phone (IVR), mobile app, smart speakers, and WhatsApp.
Step 5: Measure and iterate. Track booking completion rate, no-show rate delta, cost-per-booking reduction, and patient satisfaction scores. Use A/B testing for reminder timing, channel, and conversational style.
Conclusion
Voice assistants in healthcare do not just enhance operational efficiency. They play a vital role in advancing patient-centric care by removing friction from the first touchpoint most patients have with a hospital: booking an appointment. By automating and personalising the scheduling process, they help healthcare providers reduce administrative burden, cut no-show rates, lower cost-per-booking, and free clinical and front-desk staff to focus on higher-value interactions.
The integration of voice assistants with EHR, CRM, and telehealth platforms means the scheduling interaction becomes the starting point for a connected patient journey, not an isolated transaction.
Book a demo to see how Quad One’s AI-powered voice and scheduling solutions connect appointment booking, patient engagement, and clinical workflows in one platform.





