Hospitals are under pressure to expand access, improve patient experience scores, and operate with fewer manual steps. A modern hospital CRM ties together communications, preferences, and feedback with clinical context to make every touchpoint timely, relevant, and safe. Evidence shows that engaging patients and families improves safety and quality, and that systematic measurement via HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems) directly links experience to reputation and reimbursement.
This guide walks through how a hospital CRM works across the full patient journey, how it maps to HCAHPS domains, what interoperability looks like in practice, and how to measure what matters. Whether you are evaluating CRM platforms for the first time or looking to tighten your existing patient engagement workflows, every section below is designed to be actionable.
Key Takeaways
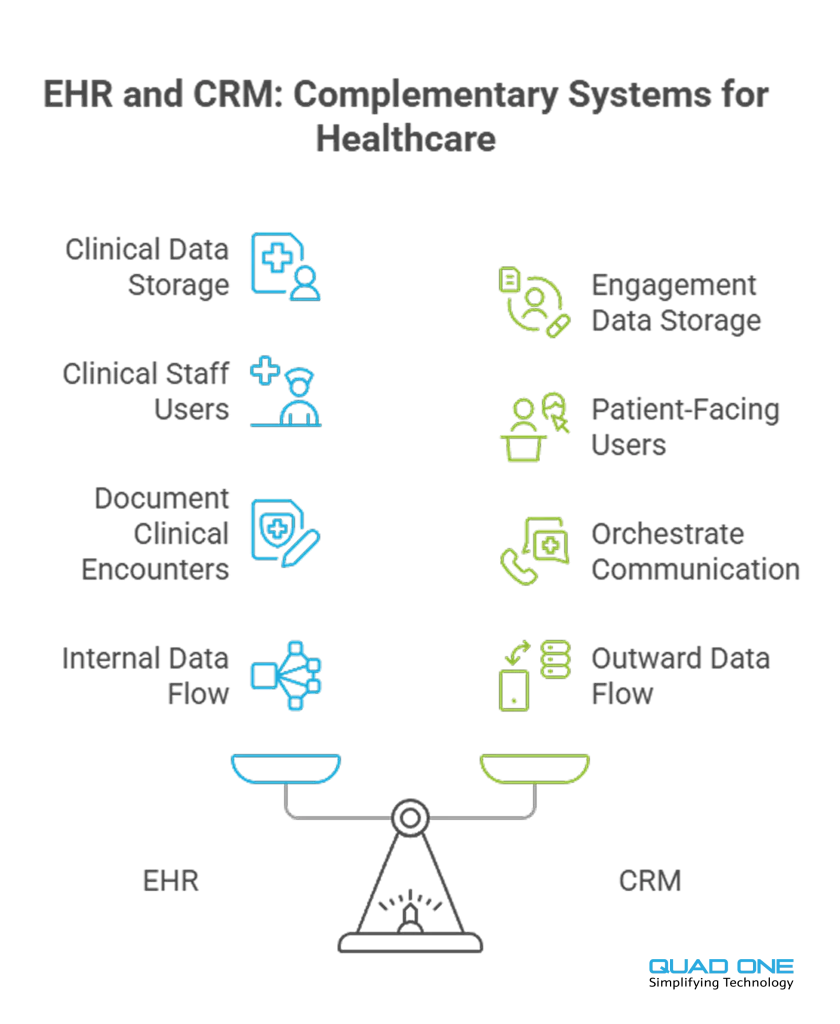
- CRM vs. EHR: The EHR is the clinical system of record. The CRM is the engagement engine that communicates and acts on that truth.
- Beyond Marketing: A hospital CRM is an operational tool for scheduling, pre-visit preparation, in-visit communication, post-discharge follow-up, and service recovery.
- Measurable Impact: The right CRM strategy delivers direct gains in no-show rates, HCAHPS scores, and referral-to-appointment times.
What Is the Difference Between a Hospital CRM and an EHR?
Think of the Electronic Health Record (EHR) as the clinical source of truth. It stores diagnoses, medications, lab results, and care plans. A hospital CRM, on the other hand, is the engagement engine that orchestrates communication and service recovery around that clinical truth.
A fit-for-purpose CRM listens for events (appointment booked, order placed, discharge complete) and triggers the right message on the right channel with full auditability. The EHR tells you what happened clinically. The CRM decides what to say, when, and how.
An AI-powered hospital CRM takes this further by using machine learning to personalize message timing, channel selection, and content based on each patient’s history and preferences.
Strong patient data management links identity, language, consents, and social context to clinical milestones. This enables personalized patient care without oversharing Protected Health Information (PHI). Omnichannel programs covering SMS, WhatsApp, email, IVR, and patient portals should be throttled by audience, timing, and sensitivity.
How Does a Hospital CRM Improve the Patient Journey?
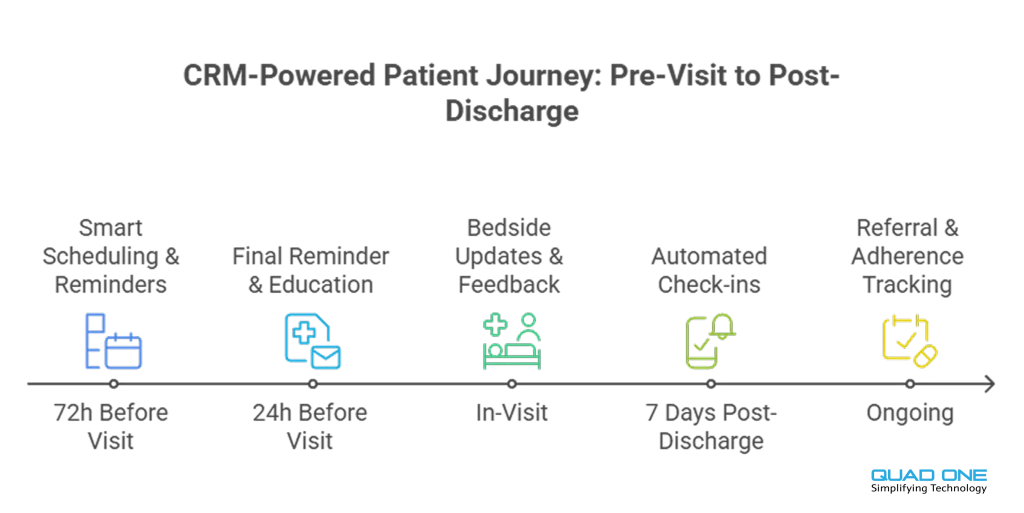
Patient journey tracking means each step, from referral received, to appointment scheduled, visit completed, and results posted, can trigger a contextual nudge. That is modern healthcare workflow automation: rules and AI work in the background so humans can focus on conversations that need a human.
Pre-Visit: Scheduling, Reminders, and Preparation
Multi-touch reminder schedules (for example, 72 hours and 24 hours before the visit) adapt when a patient confirms or reschedules. Smart waitlists auto-offer open times as they become available, matched to each patient’s channel preference. “One-tap change” links let patients who cannot make it reschedule without calling. Together, these moves reduce no-shows and late cancellations while preserving clinic capacity.
A CRM can also sequence education in plain language, capture questions ahead of time, and route special needs (such as interpreter or mobility support) to staff. These are practical CRM healthcare benefits that show up as fewer delays and better first impressions.
In-Visit: Communication and Family Engagement
Bedside updates to families, “teach-back” prompts before discharge, and role-based alerts help teams close information gaps. AHRQ’s guidance on partnering with patients and families has shown measurable improvements in safety culture and experience when applied consistently. A CRM operationalizes that playbook.
For hospitals looking to extend real-time communication beyond the facility, WhatsApp patient communication integrated with the CRM enables secure, asynchronous messaging that patients already trust and use daily.
Post-Discharge: Follow-Ups, Referrals, and Medication Adherence
Seven-day check-ins, refill reminders, and referral tracking keep momentum after discharge. WHO and AHRQ emphasize that transitions are fragile: medication discrepancies and communication failures are common. Structured follow-ups are not optional. A CRM makes these steps predictable, documented, and visible to the team responsible for closing the loop.
How Does Hospital CRM Improve HCAHPS Scores?
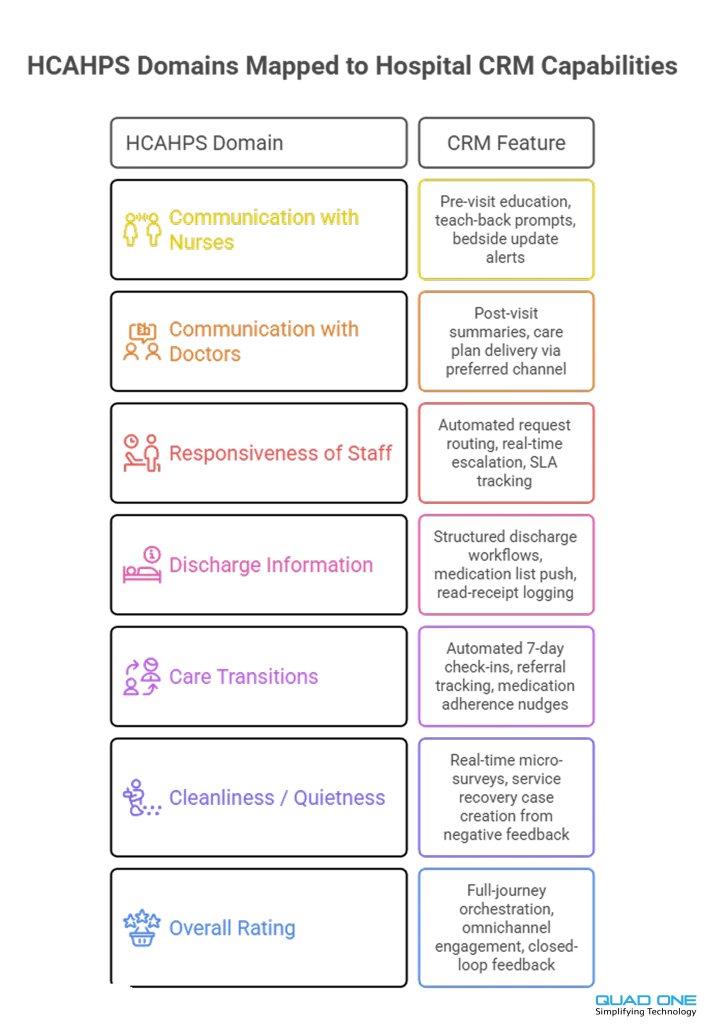
HCAHPS remains the national, standardized barometer for hospital patient experience. Scores are publicly reported and directly tied to Medicare reimbursement through the Value-Based Purchasing (VBP) program. A hospital CRM can systematically move the needle on multiple HCAHPS domains.
Communication with Nurses and Doctors: The CRM ensures pre-visit prep materials reach patients before they walk in, so clinical conversations start from a shared baseline. Post-visit summaries and teach-back prompts reinforce understanding.
Responsiveness of Hospital Staff: Automated routing of patient requests and real-time escalation alerts reduce response lag. When a patient presses a call button or submits a concern via the portal, the CRM assigns it, tracks it, and timestamps it.
Discharge Information: Structured discharge workflows push medication lists, follow-up appointments, and warning signs through the patient’s preferred channel. The CRM confirms receipt and logs read status.
Care Transitions: Post-discharge follow-up sequences, triggered automatically based on diagnosis and risk score, close the loop on referrals, medications, and home care instructions.
Hospitals investing in CRM-driven patient engagement are already seeing returns. Learn more about the future of AI in hospital CRM and how predictive analytics are being layered on top of these workflows.
How Do You Integrate Hospital CRM with EHR Using FHIR and HL7?
Interoperability standards such as HL7 and FHIR (Fast Healthcare Interoperability Resources) enable data to move safely between systems. FHIR defines resources and formats so apps, portals, and contact centers can share the same core data without brittle, one-off interfaces.
In practice, integration works through event-driven triggers. When a clinical event fires in the EHR (a new appointment, a lab result, a discharge order), the CRM receives a FHIR notification, evaluates the patient’s communication preferences and consent status, and fires the appropriate workflow. This is not a nightly batch export. It is real-time, bidirectional data flow.
Key integration touchpoints include: appointment scheduling (ADT messages via HL7 or FHIR Encounter resources), lab result availability (FHIR DiagnosticReport), discharge events (FHIR Encounter status change), and referral orders (FHIR ServiceRequest). Each touchpoint triggers a specific CRM workflow: reminders, result notifications, discharge instructions, or referral follow-ups.
The goal is a single patient record that spans clinical and engagement data. No duplicate entry, no stale information, and no manual handoffs between systems.
How Does Service Recovery Work in a Hospital CRM?
Closed-loop service recovery, acknowledging concerns, solving them, and confirming satisfaction, turns detractors into advocates. Routing and Service Level Agreements (SLAs) matter: when a low score or negative comment arrives, your CRM should create a case, assign ownership, and track resolution to protect HCAHPS domains (communication, responsiveness, discharge information, cleanliness, and more).
The workflow typically follows four steps. First, Detect: real-time micro-surveys and NPS prompts surface issues while the patient is still in the facility or within the first 48 hours post-discharge. Second, Route: the CRM assigns the case to the right department or individual based on issue type, severity, and location. Third, Resolve: the assigned owner acknowledges the concern, documents the action taken, and communicates the resolution back to the patient. Fourth, Close: the system logs the outcome, updates HCAHPS-linked dashboards, and triggers a satisfaction confirmation.
Hospitals that treat service recovery as a structured, CRM-managed process see measurably fewer negative HCAHPS responses. Patients who receive a timely acknowledgment and resolution are far less likely to rate the hospital negatively.
What Metrics Should a Hospital CRM Dashboard Track?
Dashboards must show interventions and results in the same view: reminders sent mapped to attendance delta, education sent mapped to prep completion, and recovery cases opened mapped to HCAHPS movement. That is CRM patient management with accountability.
Core metrics to track include: time to next available appointment and waitlist fill rates; HCAHPS top-box scores by domain alongside response rates to micro-surveys; patient portal and app monthly active users with completion of pre-visit tasks; service recovery throughput covering time to acknowledge and time to resolve; post-discharge follow-up completion and time to callback; referral turnaround from received to attended; and medication adherence prompts opened versus acted on.
Go beyond vanity metrics. Establish baselines and control cohorts before turning on a program. Use A/B testing for message timing, channel, and copy to continuously optimize. Systematic reviews show portals can improve patient knowledge and efficiency, but clinical endpoints are mixed without active engagement, so measure the operational steps that drive outcomes.
Compliance and Data Privacy in Hospital CRM
Modern, HIPAA-compliant CRMs enable secure texting of patient information, but this requires strict adherence to security rules, robust consent management, and audit trails. Prefer platforms that make “minimum necessary” the default, surface consent state at the moment of send, and log every access. That is how you turn policy into practice and maintain trust in patient relationship management.
An AI-powered hospital CRM with built-in compliance guardrails automates consent tracking, encrypts data at rest and in transit, and generates audit-ready reports for regulatory reviews.
Conclusion: Treat Patient Communication as Core Clinical Infrastructure
It is time to treat patient communications and service recovery as core clinical infrastructure. With the right hospital CRM, hospitals can make every touchpoint simpler and safer, align programs to national measures, and build trust at scale.
Start with targeted reminders and discharge follow-ups. Wire in feedback with SLAs. Keep expanding the playbook. The result is a smoother journey, stronger patient engagement, and a system that learns from every interaction.
Book a hospital CRM demo to see how Quad One’s AI-powered CRM connects scheduling, follow-ups, feedback loops, and HCAHPS measurement into one engagement engine.