Artificial intelligence is transforming the healthcare industry by equipping physicians with innovative tools that enhance patient treatment, simplify administrative processes, and boost patient interaction. According to Accenture, AI applications have the potential to save the US healthcare system more than $150 billion each year by 2026. With ongoing advancements in AI technology, its importance in medicine continues to grow, providing solutions that assist doctors in making quicker and more precise decisions.
But the operative word is “assist.” AI in healthcare is not replacing doctors. It is augmenting them. The most effective deployments use a human-in-the-loop model where AI recommends, generates, or flags, and clinicians verify, contextualise, and decide. This guide covers the practical ways AI is helping doctors today, the clinical applications delivering measurable results, and the framework for responsible adoption.
How Does AI Augment Physician Decision-Making Without Replacing It?
No regulatory body has approved fully autonomous clinical AI for diagnosis or treatment. Every credible clinical deployment operates on a human-in-the-loop model: AI generates a recommendation, and a licensed clinician reviews, validates, and acts on it. This is not a limitation. It is the design.
In practice, this means a radiology AI flags a suspicious lesion on a mammogram and the radiologist confirms or dismisses it. An ambient documentation tool drafts a clinical note from a patient encounter and the physician reviews and signs it. A clinical decision support system suggests a drug interaction alert and the prescribing doctor evaluates the clinical relevance.
The human-in-the-loop model works because it plays to the strengths of both parties. AI excels at pattern recognition across massive datasets, tireless monitoring, and processing speed. Doctors excel at contextual judgment, patient rapport, ethical reasoning, and handling ambiguity. Together, they produce outcomes that neither can achieve alone.
The risk is not that AI will replace doctors. The risk is that doctors who use AI will outperform those who do not, creating a competency gap. AI literacy is becoming a core clinical skill.
Key Clinical Applications of AI for Doctors (2026)
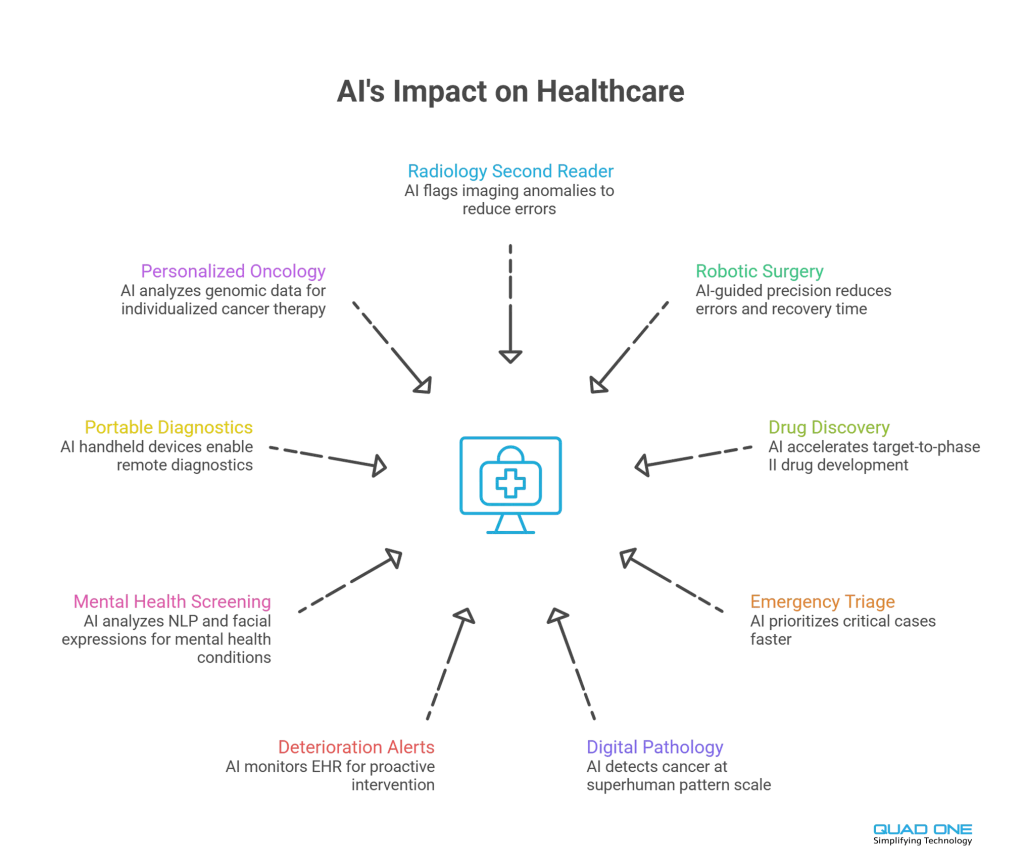
1. AI in Radiology: The Second-Reader Model
Over 70% of FDA-cleared AI tools focus on medical imaging. In radiology departments, AI operates as a “second reader”: algorithms analyse X-rays, CT scans, MRIs, and pathology slides to detect anomalies. AI algorithms have outperformed human radiologists in detecting breast cancer from mammograms. Google’s DeepMind predicts acute kidney injury up to 48 hours before onset. Hospitals report up to an 85% reduction in diagnostic errors.
2. Robotic-Assisted Surgery
AI-powered surgical robots enhance precision in complex procedures, reducing recovery time and improving patient safety. The “master-slave” model has surgeons controlling robotic arms from a console while AI provides real-time guidance, tissue identification, and movement scaling. Research shows significantly reduced intraoperative errors and postoperative complications.
3. Drug Discovery and Development
AI accelerates drug development by predicting potential drug candidates and optimising clinical trials. Insilico Medicine brought an AI-discovered candidate to Phase II trials in under 18 months. AI also enables drug repurposing, uncovering new therapeutic applications for existing compounds, reducing R&D costs by up to 60%.
4. AI in Emergency Care and Triage
AI-driven triage systems assess patient symptoms and prioritise critical cases in emergency departments, processing complaints, vitals, and history to assign acuity levels and ensure the most critical patients are seen first.
5. Digital Pathology
AI algorithms analyse pathology slides to detect cancers and rare diseases with higher accuracy than manual review, identifying patterns across thousands of cellular features simultaneously.
6. Predictive Patient Deterioration Alerts
AI monitors EHR data in real time to detect early signs of patient deterioration, analysing vital sign trends, lab results, and medication responses to flag patients whose condition is worsening before critical events.
7. Mental Health Detection
NLP and facial recognition tools identify early signs of depression, anxiety, or PTSD from patient speech patterns or expressions, supporting psychiatric screening in primary care and emergency settings.
8. AI-Enabled Portable Diagnostics
In remote or resource-limited areas, AI-equipped handheld devices (ultrasound, ECG, retinal cameras) help GPs perform accurate diagnostics without specialist support, expanding access to screening.
9. Personalised Oncology Treatment
AI models evaluate patient genetics, tumour genomics, and treatment responses to recommend individualised cancer therapies, improving efficacy and minimising side effects.
Can AI Reduce Physician Burnout and Documentation Overload?
Yes, and it is already happening at scale. Physicians spend 1–2 hours on documentation for every hour of patient care. EHR “pajama time” is a leading burnout contributor. AI addresses this through ambient clinical documentation: AI listens to the encounter (with consent), generates a structured SOAP note, and pushes it to the EHR for review and sign-off.
Tools like Nuance DAX Copilot, integrated with Epic, are deployed across major health systems. Clinicians reclaim hours per week. Documentation accuracy improves because notes are generated from the actual conversation.
Beyond documentation, AI automates prior-authorisation workflows, intelligent inbox triage, AI-generated patient communication, and pre-visit form completion.
For hospitals connecting documentation and patient communication into one layer, Quad One’s AI hospital CRM automates scheduling, follow-ups, feedback, and discharge workflows alongside clinical data.
How AI Enhances Patient Engagement and Communication
AI transforms how healthcare systems interact with patients. NLP facilitates multilingual communication. AI-based apps provide customised health recommendations, medication reminders, and instant alerts.
Quad One’s AI WhatsApp Bot enables patients to schedule, retrieve reports, and receive post-discharge instructions in their own language within WhatsApp, no app download required.
AI-powered virtual assistants provide 24/7 support, handling routine queries and performing preliminary symptom triage.
Barriers to AI Adoption in Clinical Practice and How to Overcome Them
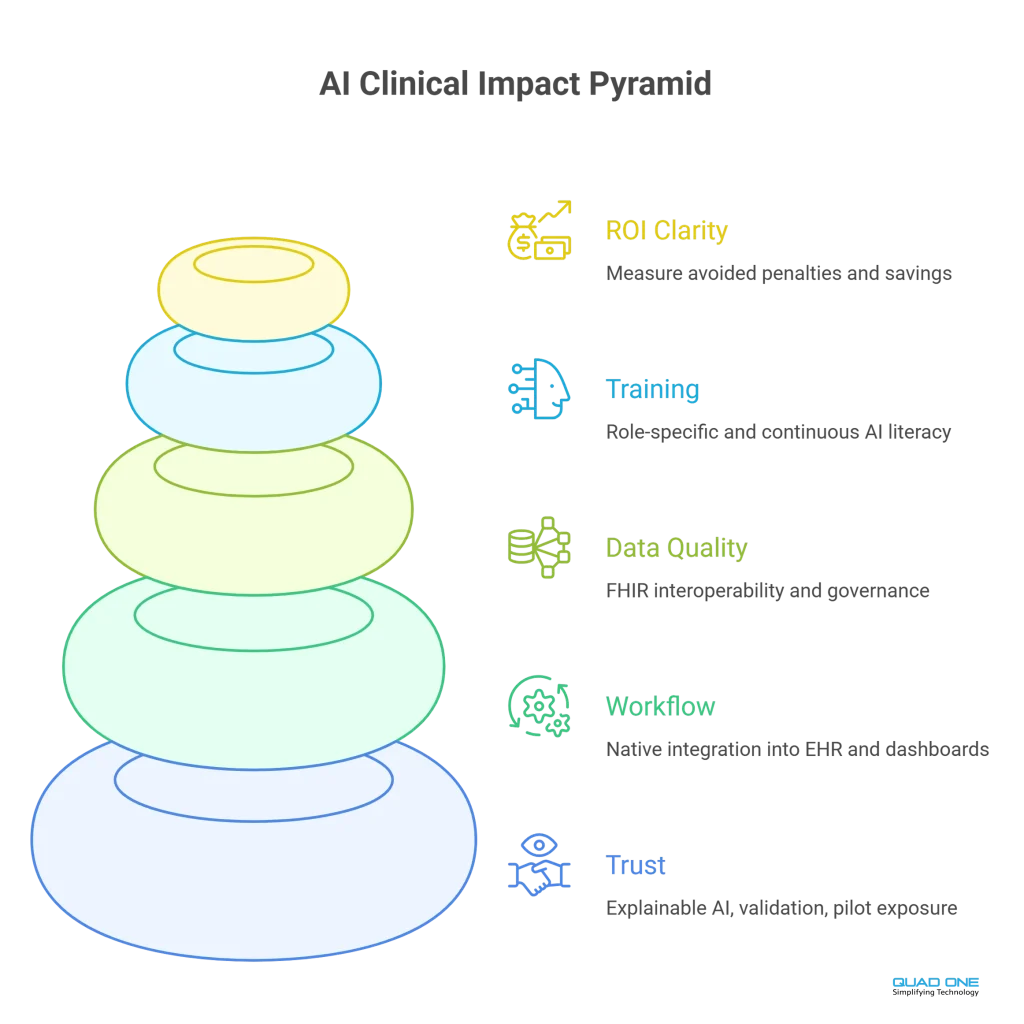
Clinician trust. Scepticism of unexplainable AI. Solution: Explainable AI, peer-reviewed validation, pilot-first exposure.
Workflow integration. Tools requiring separate interfaces see low adoption. Solution: Embed AI inside EHR, PACS, and ED dashboards natively.
Data quality and interoperability. Fragmented IT ecosystems limit AI accuracy. Solution: FHIR-based integration. Data governance before AI procurement.
Training and AI literacy. Clinicians lack training to evaluate AI outputs. Solution: Role-specific, continuous training. AI literacy as core competency.
Cost and ROI visibility. No clear financial framework. Solution: Frame ROI in avoided penalties, FTE savings, diagnostic error reduction, quality bonuses.
How Should Hospitals Measure the Clinical Impact of AI?
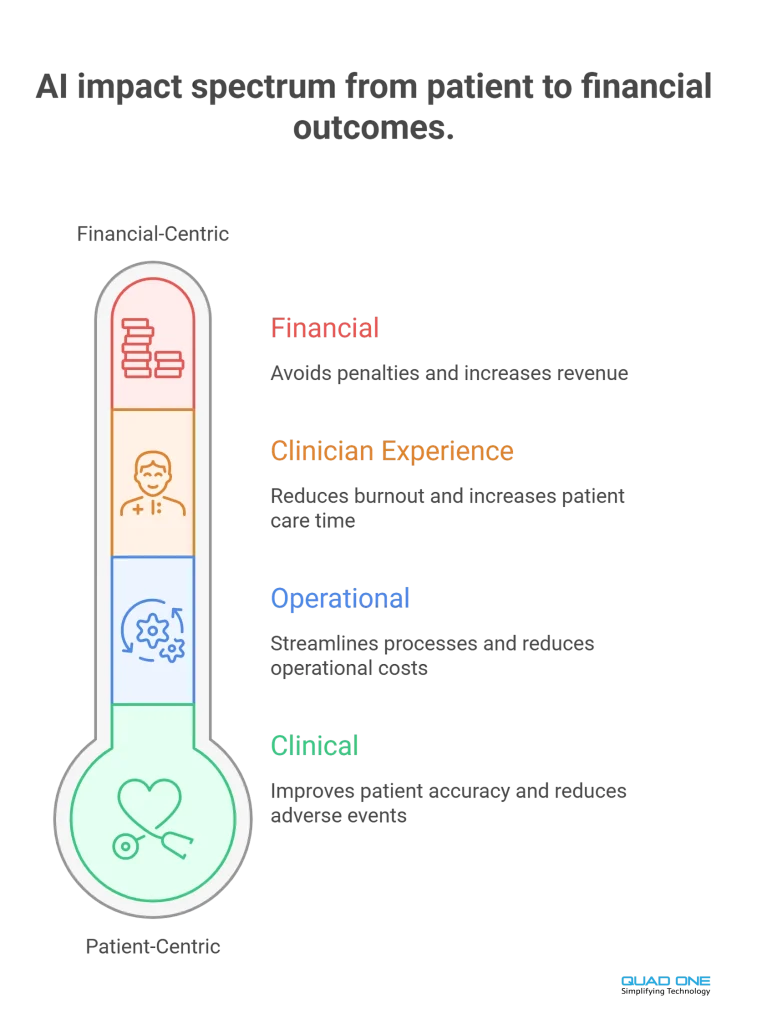
Clinical outcomes: Diagnostic accuracy (sensitivity/specificity), time-to-diagnosis, preventable adverse events, readmission rates.
Operational efficiency: Documentation time saved per clinician/day, prior-auth processing time, no-show rate delta, referral turnaround.
Financial impact: Avoided readmission penalties, malpractice cost avoidance, admin FTE savings, quality-incentive bonuses.
Clinician experience: Burnout scores (pre/post), after-hours charting reduction, direct patient care time per shift.
Use A/B testing, control cohorts, and baselines. Report outcomes, not just activity.
Ethical Considerations in AI-Doctor Collaboration
Data privacy: Every AI tool processing PHI must meet HIPAA standards: encryption, access controls, audit trails, signed BAAs.
Bias: Non-representative training datasets produce less accurate results for underrepresented populations. Require diversity audits and continuous monitoring.
Human oversight: The human-in-the-loop model must be enforced by system design and reinforced through training.
Transparency: Clinicians need to understand why an AI reached a recommendation. Black-box models face lower adoption and higher medicolegal risk.
For a deeper technical analysis of GenAI architectures and the regulatory landscape, see: Is Generative AI in Healthcare Reality or Hype?
The Future of AI in Medicine
AI-enabled blood tests and biomarkers for early disease identification from a single blood draw.
Improved robotic systems for minimally invasive surgery, including micro-robotics for targeted drug delivery.
Digital twins creating virtual patient replicas to simulate treatment outcomes before real-world application.
AI-powered clinical trial matching connecting patients to eligible trials based on genomic profile and diagnosis.
Explore Quad One’s full suite of AI in healthcare solutions connecting CRM, WhatsApp bots, and clinical workflow tools.
Conclusion
AI for doctors transforms healthcare through improved diagnostics, personalised treatments, streamlined workflows, and enhanced engagement. The hospitals that invest in AI collaboration today with proper governance, measurement, and human-in-the-loop design will define the standard of care tomorrow.
Book a demo with Quad One to see how our AI-powered platform connects diagnostics, engagement, documentation, and hospital CRM in one system.





