The healthcare sector has seen a decisive shift toward value-based care, where reimbursement hinges on patient outcomes rather than the volume of services delivered. At the centre of this shift is the AI hospital CRM, a system that goes beyond traditional patient relationship management by embedding predictive analytics, risk stratification, and automated care coordination directly into hospital workflows. For hospitals operating under value-based payment models, bundled payments, or Accountable Care Organisation (ACO) contracts, an AI-driven CRM is no longer a nice-to-have; it is operational infrastructure.
Quad One’s AI-powered hospital CRM is purpose-built for this environment, connecting clinical data, engagement workflows, and outcome measurement in a single platform.
This guide covers how AI hospital CRM improves outcomes in value-based care settings, from risk stratification and readmission reduction to personalised care plans, care coordination, ACO reporting, and measurable ROI.
Key Takeaways
- AI-driven risk stratification identifies high-risk patients before they become high-cost patients.
- Hospitals using AI hospital CRM for readmission prevention have reported up to 25% fewer chronic-disease readmissions.
- Personalised AI care plans increase patient satisfaction scores by up to 30% compared to non-personalised approaches.
- ACO and bundled-payment reporting becomes automated, not manual, when the CRM tracks outcomes natively.
- ROI materialises through lower readmission penalties, reduced administrative labour, and improved quality-incentive payments.
What Is Value-Based Care and Why Does AI Hospital CRM Matter?
Value-based care (VBC) is a reimbursement model that rewards hospitals for the quality and efficiency of care delivered, not the number of procedures performed. Under VBC contracts, including Medicare’s Hospital Value-Based Purchasing (VBP) program, bundled payments, and ACO shared-savings arrangements, hospitals earn or lose revenue based on clinical outcomes, patient satisfaction, and cost efficiency.
Traditional hospital CRMs were designed for scheduling and marketing. They lack the predictive intelligence required to manage risk, coordinate multidisciplinary care, and report outcomes at the granularity VBC demands. An AI hospital CRM closes this gap. It ingests clinical, demographic, and behavioural data; applies machine learning models for risk prediction; automates outreach and follow-up workflows; and generates audit-ready outcome reports for payer contracts.
The result: hospitals can shift from reactive care delivery to proactive population health management, which is the operational foundation of every successful VBC programme.
AI-Powered Risk Stratification: Identifying High-Risk Patients Early
Integrating AI in healthcare CRMs enhances predictive analytics capabilities, allowing providers to identify at-risk patient populations proactively. This enables timely intervention, essential in preventive care strategies, and significantly reduces hospital readmissions while improving long-term outcomes.
AI-driven algorithms analyse extensive patient data, including medical history, lifestyle factors, lab trends, social determinants, and previous hospital utilisation patterns, to predict health risks accurately. Unlike static scoring models, AI risk stratification updates dynamically as new data flows in: a patient whose blood pressure trends upward over three consecutive visits gets flagged before they present at the emergency department.
With these insights, healthcare providers can focus resources more efficiently, ensuring that the right patients receive timely preventive measures. One notable healthcare institution implemented AI-driven risk stratification through their hospital CRM, resulting in a 25% decrease in hospital readmissions for chronic diseases. This improvement was achieved by identifying high-risk patients early, delivering personalised interventions, and closely monitoring patient progress.
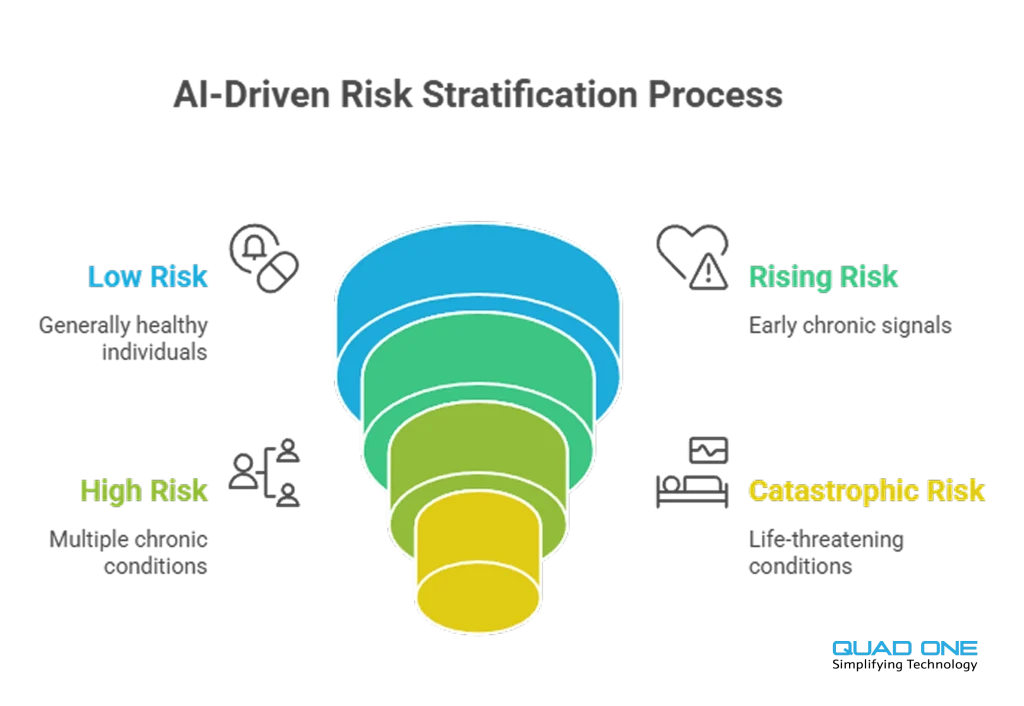
Risk tiers typically break into four groups: low-risk (healthy, preventive care focus), rising-risk (early chronic signals, early intervention), high-risk (multiple chronic conditions, coordinated ongoing care), and catastrophic-risk (life-threatening conditions, intensive specialised management). The CRM assigns care pathways and outreach cadences based on each tier.
How Does AI Hospital CRM Reduce Readmissions?
Readmission penalties under Medicare’s Hospital Readmissions Reduction Program (HRRP) cost US hospitals hundreds of millions of dollars annually. For VBC-contracted hospitals, every avoided readmission directly improves shared-savings calculations and
quality scores. AI hospital CRM attacks readmissions at three points: before discharge, during the transition window, and in the weeks that follow.
Pre-Discharge: Structured Handoff Workflows
The CRM ensures that discharge instructions, medication reconciliation summaries, and follow-up appointment details are delivered through the patient’s preferred channel before they leave the facility. Teach-back confirmation prompts verify the patient understood the plan. If confirmation is not received, the system escalates to a care coordinator.
Transition Window (0–72 Hours)
An automated 48-hour post-discharge call or message checks symptom status, medication access, and home-care setup. AI models flag patients whose responses indicate elevated re-hospitalisation risk, such as reported difficulty obtaining medications or worsening symptoms, and route them to a nurse callback queue.
Ongoing Follow-Up (7–30 Days)
Weekly automated check-ins, refill reminders, and referral-to-appointment tracking keep the patient on track. The CRM monitors whether scheduled follow-ups are attended and, if not, triggers escalation. For chronic-disease patients, the system tracks lab values and vital trends, alerting care teams to intervening deterioration before it leads to an ED visit.
For a broader view of how CRM-powered workflows operate across the full patient journey, see our guide on hospital CRM patient experience improvements.
How Do AI-Driven Personalised Care Plans Improve Outcomes?
Personalised patient care plans are becoming an essential component of value-based care. By leveraging AI insights from CRM data, hospitals can create highly tailored care plans that address individual patient needs, preferences, and health goals. These AI-driven personalised care plans enhance patient engagement, adherence to treatment, and ultimately improve healthcare outcomes.
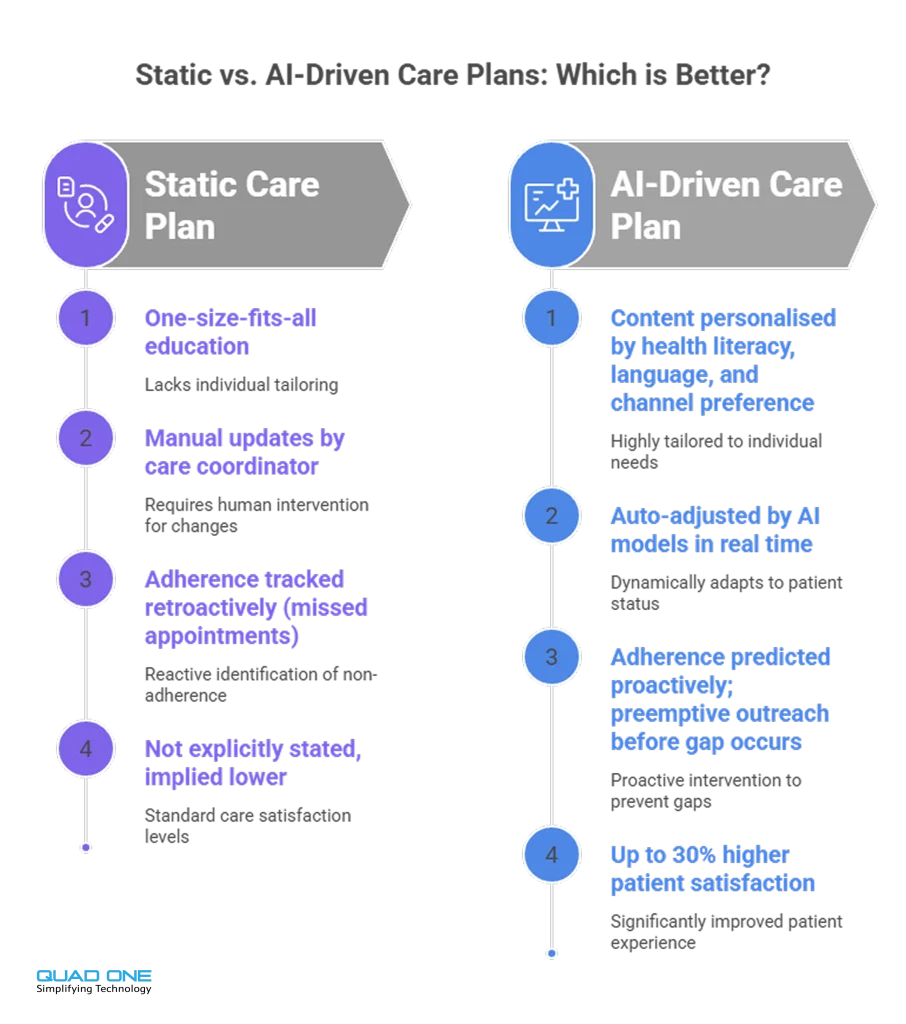
Here is how the AI layer adds value beyond what traditional care planning delivers:
Dynamic plan adjustment. Unlike static care plans written at discharge, AI-driven plans update continuously as new data arrives. A patient’s A1C result worsens? The CRM automatically adjusts outreach frequency, adds dietary education content, and alerts the endocrinologist.
Behavioural and preference modelling. The AI analyses which communication channels, message times, and content types drive the highest engagement for each patient segment. A patient who consistently ignores emails but responds to WhatsApp messages gets routed to WhatsApp automatically.
Adherence prediction. Machine learning models predict which patients are likely to fall off their care plan based on historical patterns, enabling preemptive outreach before a gap occurs rather than reactive follow-up after one.
Research indicates that personalised patient care significantly improves both satisfaction and clinical outcomes. Hospitals implementing AI-enhanced personalised care have reported up to 30% higher patient satisfaction scores compared to those without such systems.
AI-Enhanced Care Coordination Across Multidisciplinary Teams
Care coordination is critical in value-based healthcare delivery. Hospital CRMs enhanced with AI facilitate better communication and collaboration among multidisciplinary healthcare teams. Real-time data access, automated workflows, and predictive insights help reduce errors, minimise redundant tasks, and improve overall patient care quality.
In practice, this means the primary care physician, specialist, social worker, pharmacist, and care manager all see the same real-time patient dashboard. When a cardiologist updates a medication, the CRM notifies the PCP and adjusts the patient’s refill reminder sequence. When a social worker logs a housing instability flag, the system adds social-determinant-aware outreach to the care plan. No manual handoffs. No missed signals.
A leading healthcare provider utilising AI-driven CRM technology observed significant cost savings and improved patient outcomes through enhanced care coordination. With real-time updates accessible to all healthcare providers involved, redundancies were drastically reduced, patient safety improved, and costs associated with unnecessary interventions were notably diminished.
Data Analytics and Outcome Measurement in Value-Based Care
AI-enabled hospital CRMs offer robust data analytics and outcome measurement capabilities. Providers can track critical metrics such as hospital readmission rates, patient satisfaction scores, and preventive care effectiveness. This ability to systematically analyse outcomes enables continuous, data-driven improvements, aligning closely with the principles of value-based care.
Hospitals adopting AI analytics within their CRM platforms have reported substantial improvements in clinical outcomes and patient satisfaction. One healthcare network experienced a 15% improvement in clinical quality metrics within a year of AI-driven CRM implementation. Data-driven insights allowed for targeted interventions, optimised resource allocation, and improved preventive care strategies.
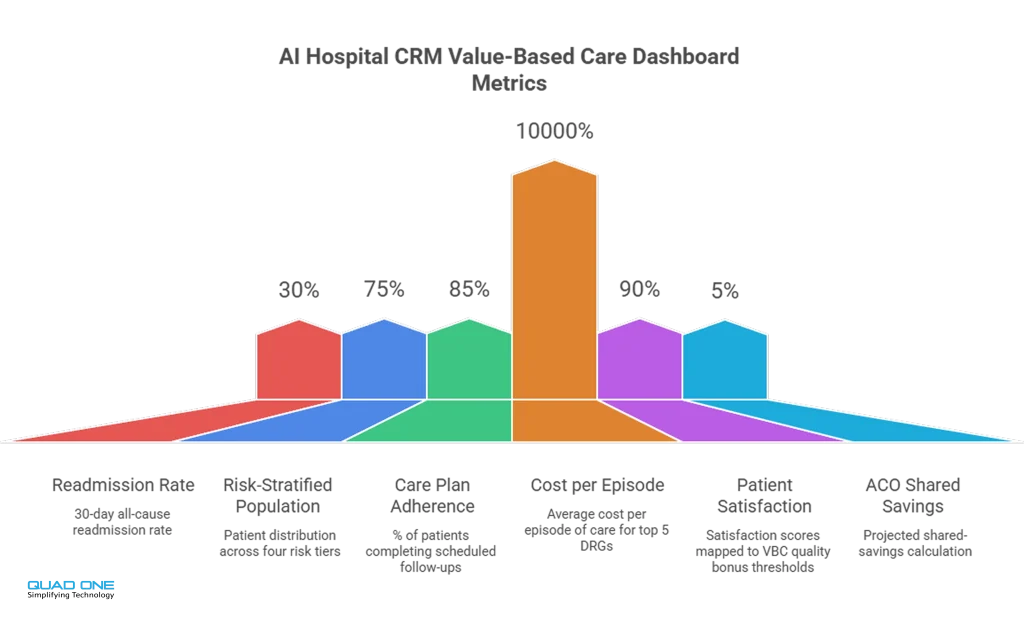
The dashboard should connect interventions to results: risk-stratified outreach volumes mapped to readmission-rate changes; care-plan adherence scores mapped to cost-per-episode trends; and referral completion rates mapped to specialist utilisation. Without this closed loop, VBC reporting is guesswork.
How AI CRM Supports ACO and Bundled-Payment Reporting
Accountable Care Organisations (ACOs) and bundled-payment programmes require hospitals to report granular outcome data to CMS and commercial payers. This includes quality measures (often drawn from CMS’s ACO quality measure set), cost benchmarks, and patient-reported outcomes. Manually compiling these reports is labour-intensive, error-prone, and typically months behind the data.
An AI hospital CRM automates this process. It continuously aggregates clinical, engagement, and cost data against the specific measures required by each contract. Quality measure numerators and denominators are calculated in real time. Gaps in care that would drag down a quality score are flagged immediately, giving care teams time to intervene before the reporting period closes.
For bundled-payment programmes, the CRM tracks cost-per-episode against the target price, alerts administrators when an episode is trending over budget, and identifies the cost drivers (unplanned readmission, extended length of stay, post-acute care utilisation). This turns VBC reporting from a retrospective compliance exercise into a prospective management tool.
Overcoming Implementation Challenges
Despite clear benefits, integrating AI into existing hospital CRM systems presents several challenges that healthcare decision-makers should address proactively.
Data integration complexity. AI models require clean, normalised data from multiple sources: EHR, claims, pharmacy, and sometimes wearables. Hospitals with fragmented IT ecosystems need an interoperability layer (FHIR-based APIs are the industry standard) to unify data before AI can deliver value.
Staff adoption. Clinicians and care coordinators need to trust AI recommendations. A phased rollout, beginning with a single high-impact use case like readmission prediction, builds confidence through visible results before expanding to broader population-health workflows.
ROI clarity. Hospital decision-makers may hesitate without a clear understanding of financial returns. Frame ROI around avoided readmission penalties, reduced administrative FTEs for manual outreach and reporting, and improved quality-incentive payments from payer contracts.
Data security. AI-driven CRM systems store vast amounts of patient data. HIPAA-compliant encryption, role-based access controls, and continuous audit logging are non-negotiable. The CRM vendor must sign a Business Associate Agreement (BAA) and demonstrate SOC 2 or equivalent security certification.
For a deeper look at where AI-driven CRM is heading, explore our piece on the future of AI in hospital CRM.
What ROI Can Hospitals Expect from AI CRM in Value-Based Care?
The financial case for AI hospital CRM in VBC environments rests on four pillars:
1. Avoided readmission penalties. Medicare’s HRRP penalises hospitals up to 3% of base DRG payments for excess readmissions. An AI CRM that reduces chronic-disease readmissions by 25% can translate to hundreds of thousands of dollars in avoided penalties for mid-sized hospitals.
2. Quality-incentive payments. Under the VBP program and ACO contracts, hospitals that hit quality thresholds earn bonus payments. AI-driven outreach that improves care-plan adherence and patient satisfaction directly boosts the quality scores that determine these payments.
3. Administrative labour savings. Automating post-discharge calls, referral follow-ups, care-gap outreach, and VBC reporting reduces the FTE burden on care coordination and quality teams. Hospitals report 20–30% better utilisation of clinical staff time after CRM automation.
4. Reduced cost per episode. Better risk stratification and proactive management keep patients out of high-cost settings (ED, inpatient). For bundled-payment contracts, lower cost-per-episode means higher margin.
AI automation reduces labour costs, minimises appointment no-shows, and increases overall hospital efficiency, leading to substantial financial returns. Hospitals should expect to see measurable ROI within 12–18 months of full deployment, with the strongest early returns in readmission avoidance and reporting automation.
Conclusion
The integration of AI in hospital CRM systems represents a transformative opportunity to enhance value-based care outcomes significantly. By improving risk stratification, delivering personalised patient care, optimising care coordination, and automating VBC reporting, hospitals can achieve better clinical outcomes, higher patient satisfaction, and greater operational efficiency.
Healthcare decision-makers must proactively embrace AI-driven CRM solutions to fully realise these benefits and meet evolving patient expectations and payer requirements.
AI-powered hospital CRM from Quad One delivers advanced patient engagement, streamlined workflows, and powerful analytics to improve healthcare outcomes in value-based care environments.
Book an AI Hospital CRM Demo to see how Quad One’s platform connects risk stratification, care coordination, and outcome reporting into one system built for value-based care.